Tracking neurological inflammation in the eyes
By imaging the eyes fundus of patients with multiple sclerosis, researchers at the Institut de la Vision have succeeded in monitoring the activity of immune cells during neuroinflammatory episodes in vivo. These results, published last December in Brain Communications, are a first step towards understanding the inflammatory mechanisms of neurodegenerative diseases in order to improve clinical diagnosis and patient management.
It is often said that the eyes are the mirror of the soul. At the Institut de la Vision, we say that the eyes are the mirror of the central nervous system. Since the optic nerve and retina are part of it, this makes the eyes extensions of the brain more than just peripherals. This particularity gives access, in a non-invasive way, to the cellular mechanisms involved in inflammation and regeneration of the nervous system to better understand neurodegenerative diseases. It is by taking this side road that Elena Gofas-Salas, INSERM research scientist in Kate Grieve's team at the Institut de la Vision, in collaboration with the Pitié-Salpêtrière Hospital and the 15-20 Hospital, has shown that by modifying the AOSLO device – an adaptive optics imaging technique – it is possible to monitor the appearance and evolution of immune cells within the layer of ganglion cells – retinal cells, one of its extensions, i.e. axons, form the optic nerve – of patients with multiple sclerosis (MS). In these initial results, the researcher highlights a definite correlation between the presence of immune cells and the appearance of optic neuritis - inflammation of the optic nerve - which is one of the most common symptoms of MS. She notes a sharp increase in the number of infiltrated cells (which do not normally belong to the retinal ecosystem) during episodes of optic neuritis and, in some cases, observes an increase in the number of these cells before the first clinical symptoms.
Probing the invisible
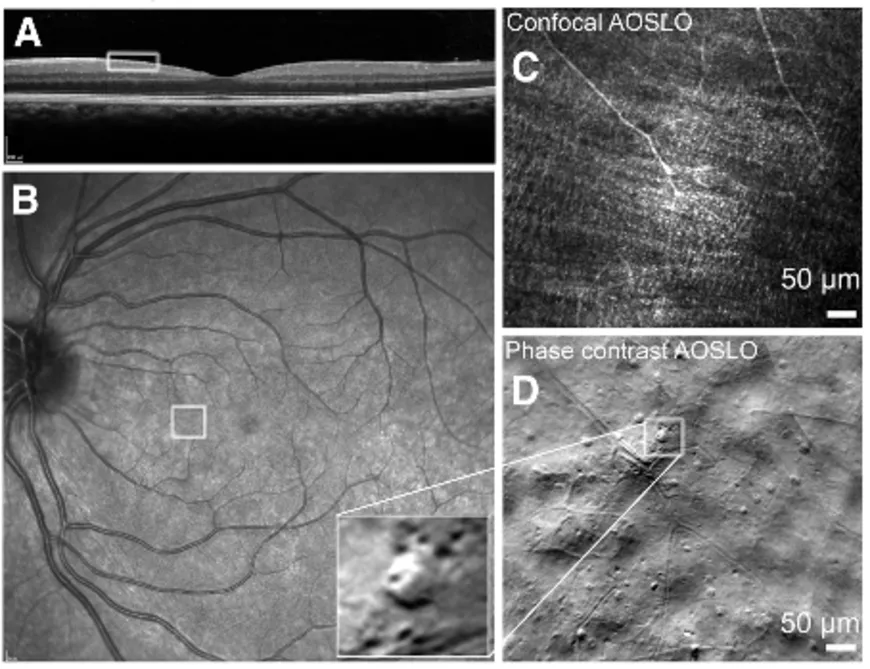
To image objects as small as immune cells, the young researcher uses an imaging device that her team employs to examine the retina: the adaptive scanning laser ophthalmoscope (AOSLO). A laser beam is directed into the eye toward the retina. It reflects off the different layers of the retina before exiting the eye. Recording the fluctuation in light intensity provides information about the retina, which is used to reconstruct the image. The acquisition is coupled with an "adaptive optics" system that corrects for image distortion caused by the beam passing through the cornea and other anterior layers of the eye. "Thanks to this correction, we can see at the cellular level - as small as two microns [one-thousandth of a millimeter]. Many inflammatory cells are between five and ten microns. in size" Elena explains. By scanning a section of the retina both on the surface and in depth, the researchers are able to obtain a very high-resolution 3D image of the retina and its constituent cells in real time.
However, immune cells are almost transparent, making them difficult to detect optically. An adjustment of the imaging device was therefore required to make it sensitive to the light deflected by the cells. "Instead of looking at how the light is reflected or absorbed, we look at how it is deflected," Elena explains. “Depending on how it is scattered, the detectors [added to the AOSLO] receive more or less light.” This part of the light, known as "off-axis" light, which is not usually used during measurements, could thus reveal the presence of immune cells within the ganglion cell layer.
"After developing the technique, we thought it would be interesting to apply this detection to patients who potentially have inflammation and therefore an activation of the immune system," the young researcher continues.
A new imaging technique tested on patients
To conduct their study, Elena and her team collaborated with the Pitié-Salpêtrière Hospital, the Paris Brain Institute and the Clinical Investigation Center (CIC) for neuroscience (led by Prof. Céline Louapre, a neurologist), which follows cohorts of MS patients, as well as with the CIC of the 15-20 Hospital, whose imaging platform was investigated the vascular alterations caused by this disease (a platform led by Prof. Michel Paques, a hospital practitioner and researcher at the Institut de la Vision).
MS is an autoimmune disease that affects the brain and spinal cord. As the leading cause of severe non-traumatic disability among young adults [1], it results of the dysfunction of the immune system, which, for unknown reasons, attacks nerve cells instead of protecting against external threats (such as viruses and bacteria) causing motor, cognitive or visual problems. Immune cells break down myelin, a biological membrane that surrounds the axons through which neurons communicate. The breakdown of the myelin sheath of the axons, which form the optic nerve, causes significant inflammation leading to a sudden and painful loss of visual acuity. This inflammation of the optic nerve, called optic neuritis, is an ideal candidate for observing potential immune activity within the retina.
"It is thanks to Professors Michel Paques and Céline Louapre that we were able to have access to the cohorts of patients. They made the link between us, the research engineers, and clinical research by putting us in contact with clinicians so that our imaging could be included in the cohort protocol," Elena says.
The introduction of AOSLO imaging in the follow-up of MS patients enabled Elena and her team to access 51 MS patients followed at the Pitié Salpêtrière Hospital.
What AOSLO imagery reveals
Through this study, the researchers aim to demonstrate that it is possible to observe the dynamics of immune cells using the AOSLO system during and after optic neuritis.
"We weren't necessarily expecting to see cell infiltration. But we saw all kind of cells that looked inflammatory in the layers of ganglion cells," Elena confirms.
The observed cells are located near the blood vessels of the retina and are mainly found in the inner layers of the retina, far from the photoreceptors. They move slowly at an estimated speed of 3.2 +/- 1 micrometers per hour and appear to move in and out of blood vessels. These movements suggest migrations and infiltrations similar to the mechanisms of immune responses during local inflammation of the retina.
In addition to confirming the presence of immune cells, the researchers were able to demonstrate a link between the concentration of these cells and the onset of optic neuritis. "There are many more infiltrating cells during and after optic neuritis. We observed this particularly in one patient who developed neuritis during the study. We noted a marked increase in the number of cells even before the clinical signs," the researcher reveals.
However, no link was found between cell concentration and the progression of optic nerve deterioration. This finding raises questions about the identification and role of the immune cells observed: what are these cells? Are they there to damage or regenerate the optic nerve?
The first morphological analyses of the cells are consistent with previous histological studies of retinal nervous tissue associated with MS. They suggest that some of the infiltrated cells observed are microglial cells and lymphocytes. In addition, other cells exhibit morphologies similar to those of macrophages and monocytes.
Despite the analyses and comparisons with the retinas of individuals without MS, it remains difficult to distinguish cells already present in the retina from cells that appear before and during an inflammatory phase.
A first step forward that raises questions
Although experimental in vivo systems already exist for monitoring immune responses in the central nervous system, they are not precise enough to detect all the biomarkers of inflammatory reactions that would guide clinical diagnoses. By applying their non-invasive imaging technique, Elena Gofas and her team have succeeded for the first time in observing and tracking in vivo the dynamics of immune cells infiltrating the human retina during inflammation. However, these biomarkers need to be precisely identified to determine the immune mechanisms activated during optic nerve inflammation.
"It's striking to observe inflammatory cells in retinal tissue that does not contain myelin, since it is located upstream of the optic nerve. This raises questions about the broader role of MS inflammation: beyond attacking myelin, how does it contribute to retinal neuronal damage?" Elena asks.
One thing is certain: by incorporating such advanced imaging techniques into cohort protocols, many other neurodegenerative diseases could be investigated.
These findings, which represent a first step towards a better understanding of neurological inflammatory mechanisms, are the result of a collaboration between clinical researchers and researchers at the Institut de la Vision. This work underlines the Institut de la Vision's expertise in developing cutting-edge technologies as well as its close ties to clinical research.
Scientific paper : Gofas-Salas, E., Mossad, M., Beigneux, Y., Norberg, N., Castro Farias, D., Vignal, C., ... & Grieve, K. (2026). In vivo characterization of a retinal cellular biomarker of inflammation in multiple sclerosis. Brain Communications, 8(1), fcaf471.
